The REFINE Project
Rosalie van Woezik explains that chronic cancer-related fatigue is common at the Helen Dowling Institute. “Already many (online) therapies were effective in reducing fatigue, but we saw that these therapies work differently for different persons. The question remained: what works best for whom?” To answer that question, the REFINE team employed the personal network theory. During their period of waiting at the HDI, daily, several times a day, patients fill in how they are feeling, using an (experience sampling) app. This data creates a network of symptoms regarding an individual patient’s fatigue. This knowledge is then used during the treatment. The practitioner, together with the patient, looks at the patient’s personal fatigue network, and this provides many insights into the coherence of the symptoms, for example. More about REFINE…
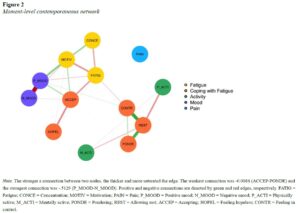
Results from qualitative research
Tom Bootsma (former PhD student at HDI, now postdoc researcher at AvL) conducted qualitative research to determine how patients experience chronic cancer-related fatigue, in order to determine: what are important nodes that belong in a network of fatigue? Bootsma also spoke with patients and their therapists about the use of the app and their experiences in practice. How did patients and their therapists experience the feedback from a personal network?
The added value in practice
Both patients and therapists saw the added value of the personal approach in the treatment of fatigue complaints at the HDI. Rosalie van Woezik: “For patients the greatest added value was that while they were waiting and filled in the app, they gained an insight into: I do indeed suffer from fatigue! That could sometimes be confrontational, but it was also necessary. It made patients realize: I have this complaint, I can do something about it, and I’m going to do something about it.” The experiences of therapists are also positive. “They were able to make the treatment more personalized. For instance, if a therapist knows at the start of the treatment that anxiety also plays a major role, he or she can use this information to make a better informed decision for the type of therapy,” says van Woezik.
The sequel: REFINE 2.0
Qualitative research shows added value, but in order to also quantitatively investigate the use of a personal network at the HDI, the project will be continued. The project has been extended with a grant from the Stichting Vrienden Integrale Oncologische Zorg (VIOZ; Friends of Integrated Oncological Care Foundation). “With REFINE 2.0 we are going to investigate what the differences are if (1) you use the personal network approach and (2) if you do not. Are there differences in outcomes?” Van Woezik explains. A group of 40 patients will complete an experience sampling (ESM) questionnaire via the app while on the HDI waiting list. They do this five times a day for 21 days and later, during the treatment, they receive feedback on their personal fatigue network based on this data. These results will be compared with the treatment as usual at the HDI. In this treatment as usual, patients complete a standard questionnaire at the intake, which also includes questions about fatigue. Van Woezik: “Qualitative research has already shown that the use of a personal network has added value, but I am curious to see whether this personalization of treatment will also be reflected in the reduction of fatigue and the burden experienced by people.”
Part of the usual care
The ultimate dream of the REFINE team is that the network approach will become part of usual care. At the Helen Dowling Institute, but also beyond. Rosalie van Woezik: “We hope that eventually, everyone on the waiting list will be able to already fill out their assessment on the app, and therefore, gain insight while waiting. I believe it can be very valuable for patients on the waiting list. I hope that, if we can demonstrate that the treatment is more focused, shorter, and more effective for those who have filled out the app, personalization treatment by using the app can eventually become available to everyone.”
Automate
To be able to apply the method on a larger scale, it is necessary to further automate or to combine everything into one large app, van Woezik thinks. “The method is quite intensive. I think there is still room for improvement as to how it could be done more efficiently, i.e., issuing questionnaires, monitoring whether someone fills out everything, and creating a personal network. We are working on how we can make it automatic so that we can also make the method feasible. We are talking to other oncology care centers to see if they would like to use the method. These experiences will help us to further develop and automatize the app to make it more feasible and more user-friendly for institutions to use.”
Input is welcome
- Do you have an idea about automatic network feedback or do you have other ideas about automation in the process?
- Do you have a similar project or experience with applying a personal network in healthcare?
The REFINE team would like to get in touch!
The timing
Patients are currently being recruited for the study, after which the study will start. The study will run until 2022.
The project team
The REFINE 2.0 team is a collaboration between the Helen Dowling Institute (HDI) and Tilburg University and consists of: Dr. Marije van der Lee (head of research HDI, endowed professor of Medical and Clinical Psychology, Tilburg University), Dr. Melanie Schellekens (post-doctoral researcher at HDI and Medical and Clinical Psychology, Tilburg University) and Rosalie van Woezik (research assistant HDI).
